Two little-known tumors, which can become cancerous, are being misdiagnosed as ADHD in kids, according to a new study out of the National Institutes of Health. Pheocromocytomas and paragangliomas are tumors, usually benign, that grow in or around the adrenal gland and secrete a range of stimulant chemicals, potentially mimicking the symptoms of Attention Deficit Hyperactivity Disorder.
Over 20% Of Children With Rare Endocrine Tumors Misdiagnosed
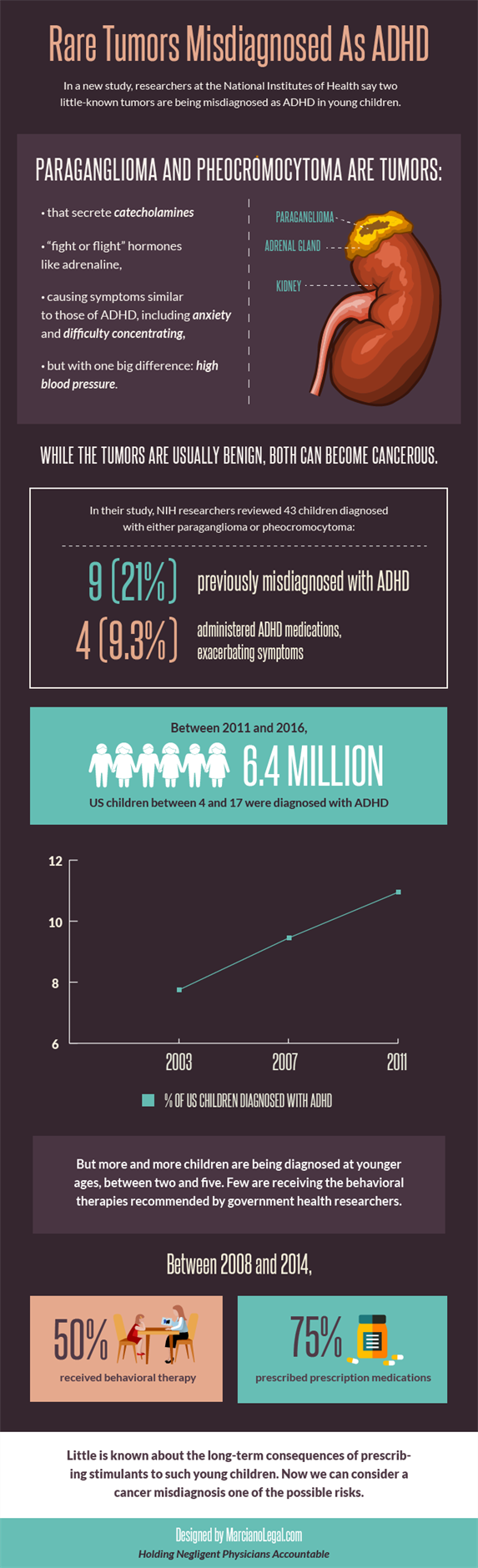
In their study, researchers at the NIH evaluated 43 children who had been diagnosed with either one of the two adrenal gland tumors between January 2006 and May 2014. Reviewing health records, scientists discovered that more than 20% of the kids had been initially misdiagnosed with ADHD, a neurodevelopmental disorder that can cause symptoms associated with inattention and impulsivity.
Of the nine total children misdiagnosed, four had been placed on ADHD medications, stimulants like amphetamine and methylphenidate, which had caused serious adverse effects, including headaches, excessive sweating and hypertension. In three of these children, the symptoms incorrectly considered related to ADHD resolved entirely after the tumors were properly identified and removed.
The researchers suggested ruling out the possibility of pheocromocytomas and paragangliomas before diagnosing children based on the common symptomatology of ADHD. Per their analysis, “symptoms of anxiety and difficulty in concentration in these patients may have been related to their underlying [pheocromocytoma or paraganglioma] and were not recognized as part of the constellation of symptoms in a child with [pheocromocytoma or paraganglioma].” Hypertension, the researchers suggest, should be a key warning sign that children who appear to have ADHD may have actually developed one of the two adrenal tumors.
The study, titled “Attention Deficit Hyperactivity Disorder in Pediatric Patients with Phecromocytoma and Paraganglioma,” was published on May 12, 2016 by the journal Hormone and Metabolic Research.
Adrenal Gland Tumors: Paraganglioma & Pheocromocytoma
Pheocromocytoma and paraganglioma are not themselves “childhood” cancers. In fact, most cases aren’t even cancerous. But statistics on the true incidence of these disorders vary widely. In their study, the NIH researchers report that around 1 in 2,500 to 6,500 patients will be diagnosed with either type of tumor. Experts at Columbia University present a far lower prevalence, at about 2 in 1 million patients. The tumors are exceedingly rare, however, by any account.
Most of the growths (or “neoplasms”) develop in people between the ages of 40 and 60. Only 10% of patients who develop pheocromocytoma or paraganglioma are children, and the conditions are associated with a genetic syndrome in around 25% of cases.So far, researchers have identified 10 different genes that can mutate and cause pheocromocytoma, although only three of those mutations are defined by the condition’s classical description.
Unfortunately, no known risk factors have been suggested for either tumor beyond the presence of certain genetic syndromes, which makes predicting who will develop the conditions nearly impossible. Perhaps this is why some doctors have dubbed paraganglioma the “pharmacologic time bomb.”
Cause & Symptoms
While both tumors involve similar types of body tissue, only one, pheocromocytomas, develop specifically in adrenal glands. The human body is equipped with two adrenal glands, found directly above the kidneys. These are endocrineglands, which means they produce hormones and secrete the chemicals into the bloodstream. Pheocromocytomas begin in a group of specialized “chromaffin” cells, responsible for producing “fight-or-flight” hormones like adrenaline, at the center of an adrenal gland. While not necessarily cancerous, the tumor can increase the production of stimulatory hormones, leading to:
- high blood pressure
- rapid or abnormally powerful heartbeat
- extreme sweating
- serious headaches
- tremors
- pale facial appearance
- shortness of breath
Symptoms of the tumor, according to the Mayo Clinic, generally “occur in brief spells of 15 to 20 minutes.” Stimulants, like those commonly used to treat ADHD, can trigger the spells, as can foods, like sauerkraut and avocado, that are high in tyramine, a substance known to increase blood pressure.
Paragangliomas, on the other hand, form outside an adrenal gland, at times alongside the carotid arteries, two large blood vessels that supply blood to the brain. Much like a pheocromocytoma, paragangliomas can produce “catecholamines,” the class of hormones implicated in stress response and blood pressure regulation, causing symptoms.
Can We Treat Tumors Of The Adrenal Gland?
Yes. When properly diagnosed, most paragangliomas can be surgically removed before severe complications occur.
In the vast majority of cases, neither pheocromocytomas nor paragangliomas acquire the ability to metastasize; various sources report that only around 3% of the tumors will become cancerous. It’s very hard, though, to tell the difference between a benign and malignant tumor through biopsy. For most patients, evidence of metastasis is likely the only way to determine that a paraganglioma or pheocromocytoma has turned into cancer.
Rising ADHD Drug Prescription Raises Concerns
American doctors are increasingly treating young children with ADHD by prescribing pharmaceuticals, despite federal recommendations that health care providers attempt behavioral therapies prior to medications.
In a recent analysis, the Centers for Disease Control and Prevention found that less than half of kids diagnosed with ADHD are receiving behavioral therapies, while nearly 75% have been placed on drugs like Adderall and Ritalin. Many insurance companies cover pills, but few are willing to reimburse families for sessions of behavioral therapy, making the recommended first-line treatment extremely costly.
Overall, ADHD diagnoses are rising rapidly. In 2003, around 7.8% of children between the ages of 4 and 17 had been diagnosed with ADHD. By 2007, that proportion had increased to 9.5%, and in 2011 it jumped again to 11%. But we’re also diagnosing ADHD at much younger ages, when government officials say behavioral therapies can have the most benefit. Just one decade ago, many doctors felt uncomfortable diagnosing children between the ages of 2 and 5 with ADHD, since distinguishing between an exuberant toddler and a patient with the biological condition can be hard. That perception has changed, dramatically. Today around one out of every three children with ADHD was diagnosed under the age of five, according to the Washington Post.
Behavioral therapies usually take months before parents and doctors can see an improvement, while medications often have an impact immediately. The long-term consequences of prescribing stimulants at a young age, however, are almost entirely unknown. Thanks to new research from the National Institutes of Health, we can now list a possible cancer misdiagnosis as just one more risk of being overeager in prescribing ADHD medications.



